Understanding corneal erosions
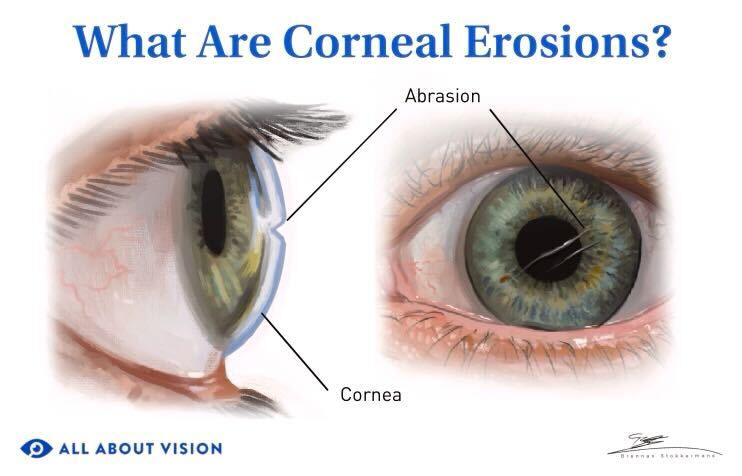
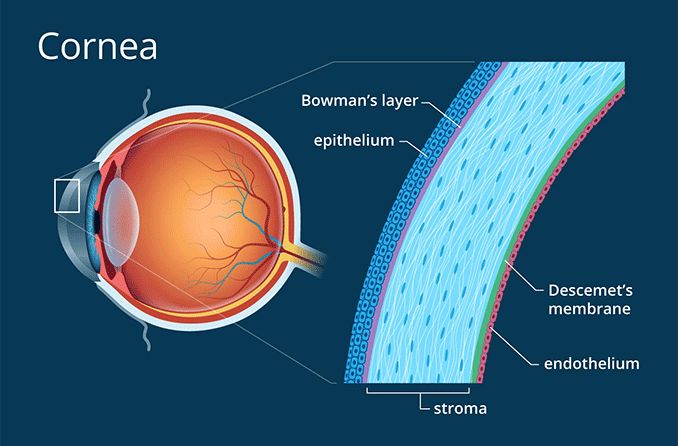
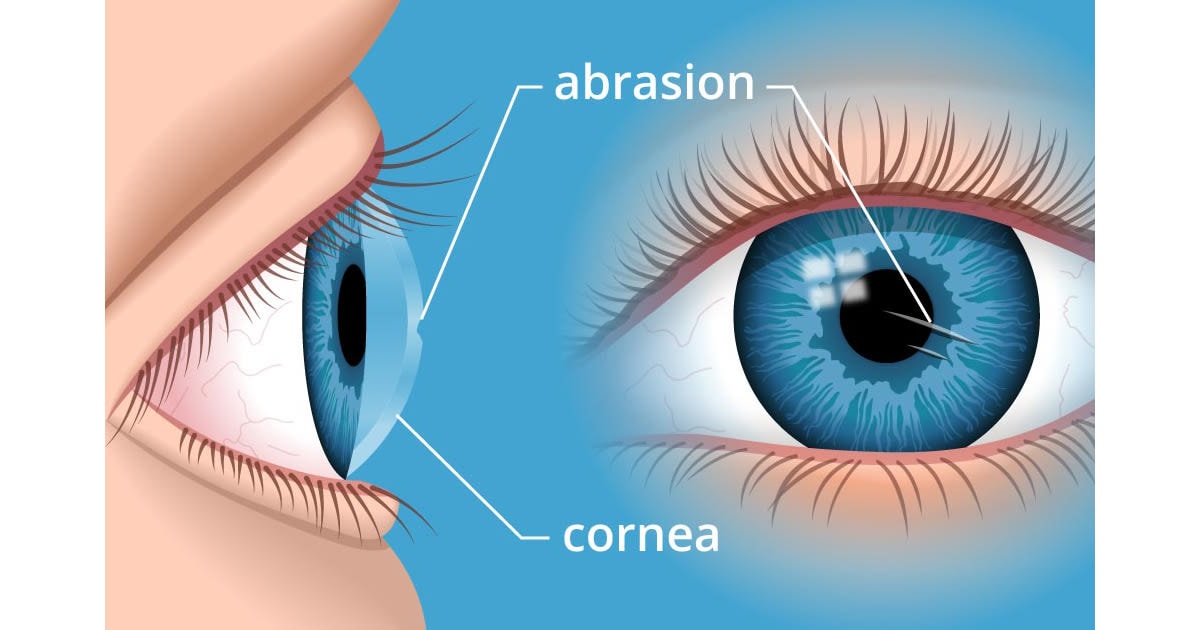
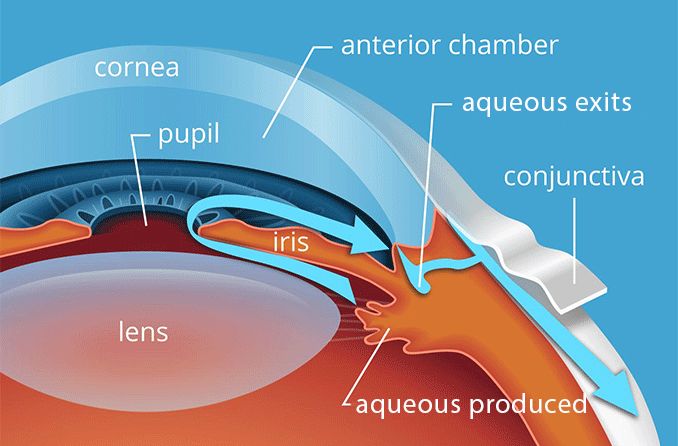
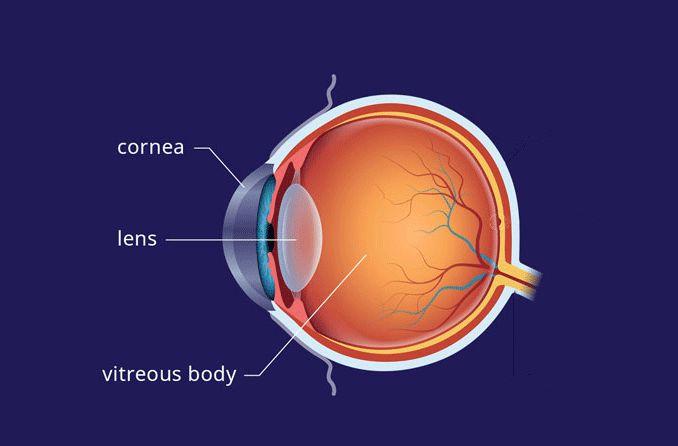
A corneal erosion happens when the top layer of the cornea (the epithelium) comes loose and pulls away from the Bowman's layer underneath. The cornea is the clear multilayered dome at the front of the eye. It's very sensitive, so even a small erosion can be painful.
Erosions typically occur in one eye, but can affect both eyes depending on the cause. They usually result from an underlying problem. Previous corneal abrasions (eye scratches) and other eye injuries are common causes.
A mild erosion may heal on its own within a few days. A more severely eroded cornea needs to be treated by an optometrist or ophthalmologist.
Recurrent corneal erosion (RCE)
Some erosions come back one or more times after they heal. This is known as a recurrent corneal erosion, or RCE. It may also be called recurrent corneal erosion syndrome (RCES) or recurrent corneal epithelial erosion syndrome.
Following a five-year study of emergency patients at a London, UK, specialty eye hospital, researchers determined an RCE prevalence rate of just under 1%.
While that may seem like a low number, it indicates that recurrent corneal erosions are not uncommon. And, since many patients recover without clinical intervention, it’s likely that not all cases are reported (or diagnosed).
Talk to an eye doctor any time you have new eye pain or sensitivity. They can assess your symptoms and provide necessary treatment to help prevent complications and future erosions.

Symptoms
Corneal erosion symptoms often start right after you wake up. This is because your eyes dry out and stick to your eyelids while you sleep. Then, when you open your eyes in the morning, the cornea’s weakened epithelial cells may peel off (or erode away) from the Bowman’s layer.
Symptoms of a corneal erosion can include:
- Eye pain that ranges from mild to severe
- Epiphora (excess eye watering)
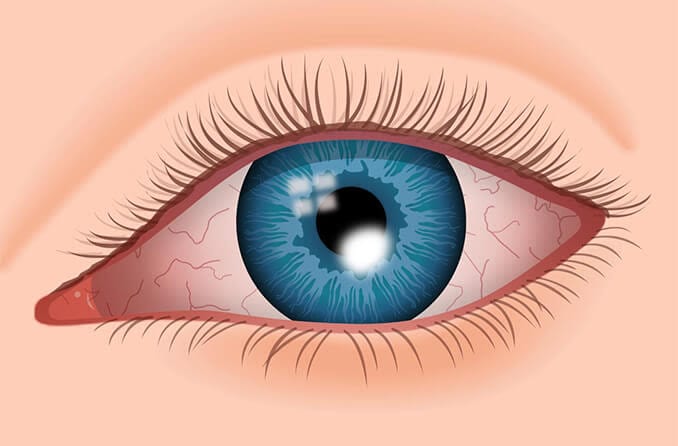
- Eye redness
- Hazy or blurry vision
- Sensitivity to light
- The feeling that something is stuck in your eye
The symptoms usually improve during the day, but they might come back the next morning. If this happens, the cycle can last several days (or longer in severe cases) before the erosion heals. Contact your eye doctor if experience ongoing eye pain or other eye issues.
READ MORE: How to stop watery eyes
Causes of corneal erosions
Corneal erosions are caused by conditions and injuries that make the cornea's outer layer (the corneal epithelium) detach more easily from the layer underneath (the Bowman's membrane). This process can expose sensitive nerve endings and be very painful.
Common causes
Common causes of corneal erosions are:
- Past corneal abrasion – The injury heals but leaves the outer part of the cornea a bit weaker than it used to be. Studies show that abrasions cause around half of all cases of RCE.
- Corneal dystrophy – These eye conditions can cause changes to your cornea over time. Around two to three of every 10 people with RCE have some type of corneal dystrophy. Epithelial basement membrane dystrophy (EBMD) is one type that often leads to erosions. It's also called map-dot-fingerprint dystrophy.
- Dry eye disease – When you don't produce enough tears or the right quality of tears to keep your eyes comfortable.
These problems may be related to each other or another eye or health condition. Your eye doctor will talk to you about your medical and family history during your exam.
Risk factors
Some conditions change how well the top layer of the cornea sticks to the layers below it. They can make it loose or weak. If the cornea’s top layer separates from the layers below, it causes corneal erosion.
The following issues and conditions may raise your risk of developing a corneal erosion:
- A previous corneal erosion
- A previous corneal abrasion or corneal ulcer
- Injury to the eye
- A form of corneal dystrophy or other disease that affects your cornea
- Dry eyes
- Past eye surgeries
- Blepharitis (a type of eyelid inflammation)
- Meibomian gland dysfunction (a problem with your eyelids' oil glands)
- Ocular rosacea
- Diabetes
- Nocturnal lagophthalmos (sleeping with your eyes open)
Diagnosis
An eye doctor can check for corneal erosions during a comprehensive eye exam.
A fluorescein eye stain test is a common way to diagnose erosions. The test doesn't hurt, but you might feel a slight scratching or stinging sensation for a moment.
The test can start in one of two ways:
- The doctor places a thin piece of paper on your eye and asks you to blink a few times. This spreads orange fluorescein dye across the surface of your eye.
- The doctor places fluorescein eye drops onto your eye and asks you to blink.
If your cornea is healthy, the dye will stay on the surface of your eye until your tear film washes it away. But if the cornea is damaged, the dye will flow through any breaks in the outer surface and build up in deeper layers.
After the dye is in place, your eye doctor will shine a blue light onto your eye. The blue light makes the orange dye glow green in the damaged areas where it accumulated. This makes it very easy to spot erosions or other problems in the cornea.
Treatment options
Treating an erosion of the cornea early can help you avoid complications and prevent more erosions in the future. Treatment may involve:
Medical therapy
For an active erosion, your eye doctor may recommend one or more of these treatments to help with pain and healing:
- Lubricating eye drops – Dry-eye drops and ointments may make blinking more comfortable. Artificial tears can be especially helpful when applied to the still-closed eyelid upon awakening. Some of the tears will reach the eye’s surface, making it much less likely that the dry inner-eyelid will scratch the eye.
- Anti-inflammatory medicine – Your doctor may recommend medicated eye drops or oral medication to reduce eye-related inflammation.
- Antibiotic eye drops – Medicated drops that help treat or prevent a bacterial eye infection.
- Cycloplegic eye drops – You may be given these drops to dilate your pupils. They work by temporarily relaxing the muscles in your eyes and may help with pain.
- Bandage contact lens – This soft lens acts as a barrier between your eye and eyelid, which can help relieve discomfort and help you heal more quickly.
- Patching – A temporary eye patch may be considered for some patients, but in most cases, patching is not recommended.
If you have recurrent corneal erosion (RCE), your eye doctor may suggest some additional techniques to prevent the future episodes. These may include:
- Oral doxycycline – Often used in combination with topical corticosteroids, doxycycline can be effective at treating and preventing recurring erosions.
- Serum tears – These eye drops are custom-made to treat severe dry eye disease using the liquid part of your blood.
- Cyclosporine eye drops – These medicated drops reduce swelling so your eyes can make more tears.
- Hypertonic ointment – This salt-based eye drop lowers swelling by drawing fluid out of the cornea.
Surgical interventions
An eye procedure may be needed when someone with recurrent corneal erosion does not respond well to other treatments. The doctor may recommend:
- Punctal plugs – These small plugs are inserted into the tear ducts to keep more moisture on the eye's surface. Some dissolve within a week or so, but others last much longer. Punctal plugs are only used for people with dry eyes, but relieving the dryness could help prevent erosions.
- Anterior stromal puncture (ASP) – Tiny holes are made on the cornea to help the outer layer stick to the Bowman’s layer below. It's often used for injury-related erosions.
- Diamond burr superficial keratectomy – This special tool is used to remove damaged tissue from the cornea. It tends to be used for erosions caused by corneal diseases such as EBMD.
- Phototherapeutic keratectomy (PTK) – This procedure uses a laser to smooth out the front of the cornea. This removes the damaged tissue that could be causing RCE. This option is typically only used when other treatments aren't very effective.
Preventive measures
Regular use of lubricating eye drops or ointments — especially upon awakening — is often the best way to prevent RCE. But if ocular lubricants like these aren't enough, your doctor may want to consider another technique.
For example, the combination of topical steroids with oral doxycycline has helped many patients prevent or reduce the occurrence of future erosions. Other preventive options could include some of the treatment methods listed earlier.
READ MORE: How to prevent eye injuries
Potential complications
Many corneal erosions are complications themselves because they resulted from a separate problem. It’s rare for erosions to cause their own complications.
The most common complication of an erosion is that it comes back repeatedly (a recurrent corneal erosion). It can also lead to:
- Eye infections
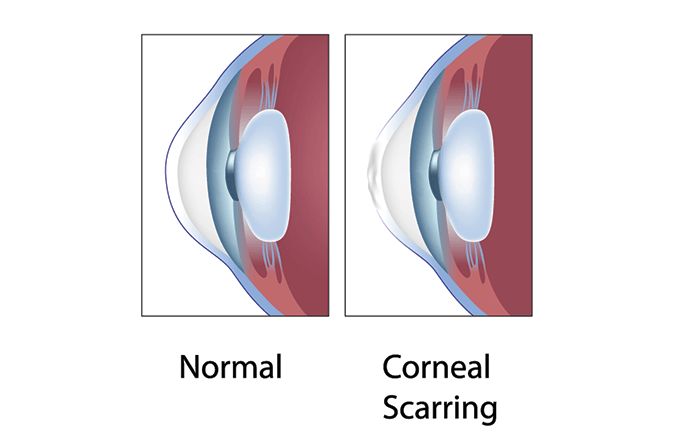
- Corneal scars that could make the cornea appear hazy
- Reduced vision
Your eye doctor can talk to you about your specific risks and complications during your appointment.
Living with corneal erosions
While corneal erosions can be painful and frustrating, minor cases often heal quickly on their own. Recurrent erosions are more likely to need medical care, but serious complications are rare. An eye doctor can assess your condition, provide treatment and help you take steps toward prevention.
Schedule an eye exam if you think you have a corneal erosion or other eye problem. Early diagnosis and treatment can help prevent future problems and protect your vision.