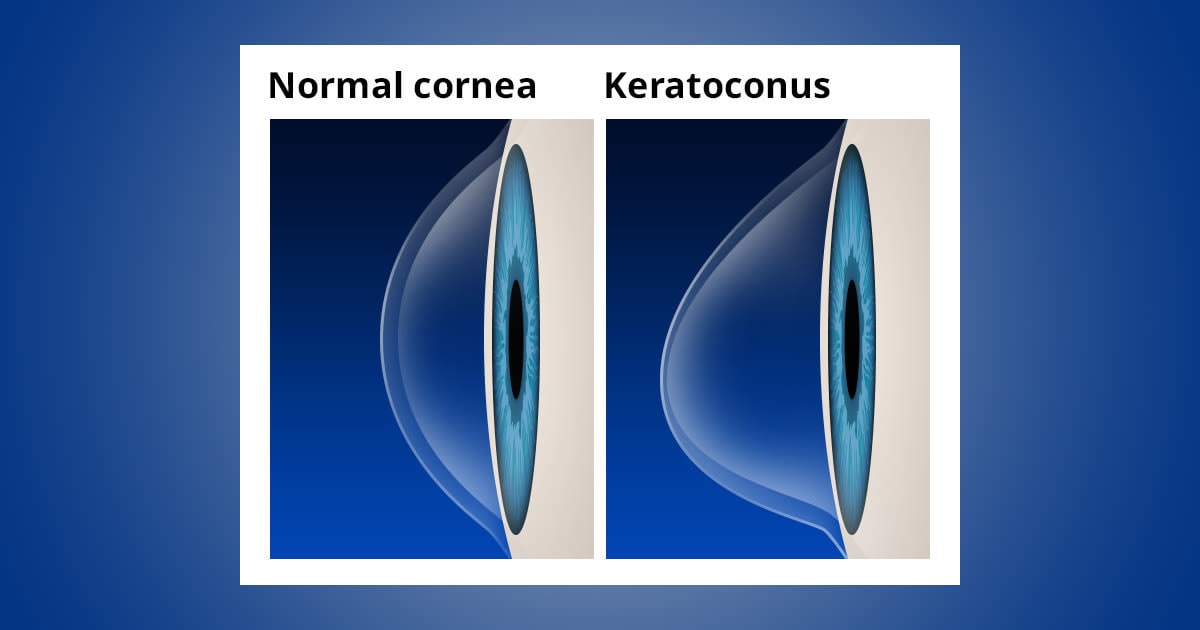
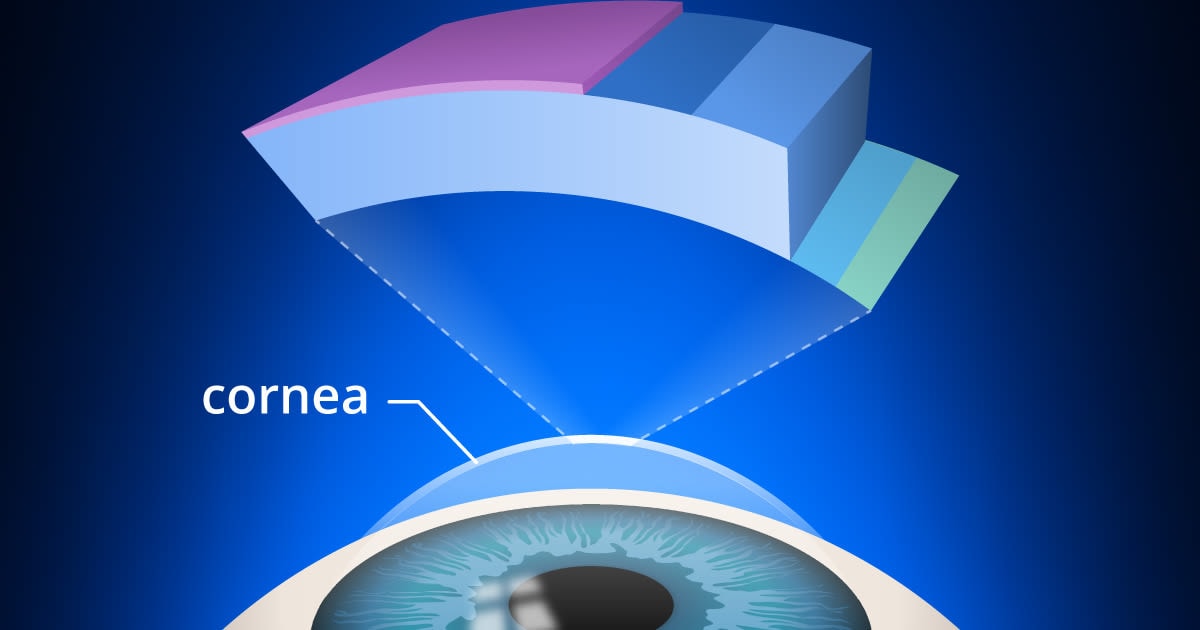
Keratoconus signs and symptoms
As the cornea becomes more irregular in shape, it causes progressive myopia and irregular astigmatism to develop, creating additional problems with distorted and blurred vision. Glare and light sensitivity also may occur.
Often, keratoconic patients experience changes in their eyeglass prescription every time they visit their eye doctor.
What causes keratoconus?
Research suggests the weakening of the corneal tissue that leads to keratoconus may be due to an imbalance of enzymes within the cornea. This imbalance makes the cornea more susceptible to oxidative damage from compounds called free radicals, causing it to weaken and bulge forward.
Risk factors for oxidative damage and weakening of the cornea include a genetic predisposition, explaining why keratoconus often affects more than one member of the same family.
Keratoconus also is associated with overexposure to ultraviolet rays from the sun, excessive eye rubbing, a history of poorly fitted contact lenses and chronic eye irritation.
Keratoconus treatment
In the mildest form of keratoconus, eyeglasses or soft contact lenses may help. But as the disease progresses and the cornea thins and becomes increasingly more irregular in shape, glasses and regular soft contact lens designs no longer provide adequate vision correction.
Treatments for progressive keratoconus include:
1. Corneal crosslinking
This procedure, also called corneal collagen cross-linking or CXL, strengthens corneal tissue to halt bulging of the eye's surface in keratoconus.
The aim of corneal cross-linking is to strengthen the cornea by increasing the number of "anchors" that bond collagen fibers together. (Diagram: Boxer Wachler Vision Institute)
There are two versions of corneal crosslinking: epithelium-off and epithelium-on.
With epithelium-off crosslinking, the outer layer of the cornea (called the epithelium) is removed to allow entry of riboflavin, a type of B vitamin, into the cornea, which then is activated with UV light.
With the epithelium-on method (also called transepithelial crosslinking), the corneal epithelium is left intact during the treatment. Advantages include less risk of infection, less discomfort and one-day visual recovery.
Currently, the only corneal cross-linking platform that is FDA-approved for the treatment of progressive keratoconus in the U.S. is epithelium-off cross-linking performed with a Glaukos KXL System and proprietary Photrexa and Photrexa Viscous riboflavin solutions. (Glaukos recently acquired Avedro.)
The use of any drug or drugs other than Photrexa Viscous and Photrexa or any device other than the KXL System for corneal cross-linking is not FDA approved, except as part of an investigational new drug study.
Corneal crosslinking may reduce significantly the need for corneal transplants among keratoconus patients. It also is being investigated as a way to treat or prevent complications following LASIK or other vision correction surgery.
Using a combination of corneal crosslinking and Intacs implants also has demonstrated promising results for treating keratoconus. Also, progressive mild to moderate keratoconus has been safely and successfully treated with a combination of corneal crosslinking and implantation of a toric phakic IOL.
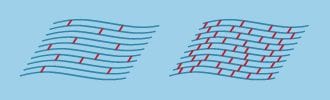
The aim of corneal cross-linking is to strengthen the cornea by increasing the number of "anchors" that bond collagen fibers together. (Diagram: Boxer Wachler Vision Institute)
2. Custom soft contact lenses
Recently, contact lens manufacturers have introduced custom soft contact lenses specially designed to correct mild-to-moderate keratoconus. These lenses are made-to-order based on detailed measurements of the person's keratoconic eye(s) and may be more comfortable than gas permeable lenses (GPs) or hybrid contact lenses for some wearers.
In the United States, custom soft contacts that are available for the correction of keratoconus include:
- KeraSoft lenses (Bausch + Lomb). These high-water silicone hydrogel lenses can correct up to 20 (D) of nearsightedness or farsightedness and up to -12 D of astigmatism.
- NovaKone lenses (Bausch + Lomb). These medium-water hydrogel lenses can correct up to 30 D of nearsightedness or farsightedness and up to -10 D of astigmatism.
Both lenses have a very wide range of fitting parameters for a customized fit and are larger in diameter than regular soft lenses for greater stability on a keratoconic eye.
Custom toric soft contacts for keratoconus are significantly more expensive than regular soft contacts, but vision insurance may cover some of the costs associated with contact lenses for keratoconus.
3. Gas permeable contact lenses
Because eyeglasses and soft contact lenses often cannot provide adequate visual acuity in cases of keratoconus, gas permeable contact lenses usually are the preferred treatment. GP lenses vault over the cornea, replacing its irregular shape with a smooth, uniform refracting surface to improve vision.
Fitting contact lenses on an eye with keratoconus often is challenging and time-consuming. You can expect frequent return visits to your eye care provider so he or she can fine-tune the fit and your prescription, especially if your keratoconus continues to progress.
4. "Piggybacking" contact lenses
Because fitting a gas permeable contact lens over a cone-shaped cornea can sometimes be uncomfortable for a person with keratoconus, some eye care practitioners advocate "piggybacking" two different types of contact lenses on the same eye.
For keratoconus, this method involves placing a soft contact lens, such as one made of silicone hydrogel, over the eye and then fitting a GP lens over the soft lens. This approach increases wearer comfort because the soft lens acts like a cushioning pad under the rigid GP lens.
Your eye care practitioner will monitor closely the fitting of "piggyback" contact lenses to make sure enough oxygen reaches the surface of your eye, which can be a problem when two lenses are worn on the same eye. However, most modern contacts — both GP and soft — typically have adequate oxygen permeability for a safe "piggyback" fit.
5. Hybrid contact lenses
The UltraHealth and ClearKone hybrid contact lenses manufactured by SynergEyes combine a highly oxygen-permeable rigid center with a soft peripheral "skirt." These lenses were designed specifically for keratoconus, and the central GP zone of the lens vaults over the cone-shaped cornea for increased comfort.
Hybrid contact lenses provide the crisp optics of a gas permeable contact lens and wearing comfort that rivals that of soft lenses, according to SynergEyes. UltraHealth and ClearKone are available in a wide variety of parameters to provide a fit that conforms well to the irregular shape of a keratoconic eye.
6. Scleral and semi-scleral lenses
These are large-diameter gas permeable contacts — large enough that the periphery and edge of the lens rest on the "white" of the eye (sclera).
Scleral lenses cover a larger portion of the sclera, whereas semi-scleral lenses cover a smaller area.
Because the center of scleral and semi-scleral lenses vaults over the irregularly shaped cornea, these lenses don't apply pressure to the eye's cone-shaped surface for a more comfortable fit.
These larger lenses also are more stable than conventional gas permeable contact lenses, which move with each blink because they cover only a portion of the cornea.
7. Prosthetic lenses
Eyes with advanced keratoconus may require an advanced prosthetic scleral lens design.
One example are lenses made with the EyePrintPRO process (EyePrint Prosthetics). This system uses proprietary Elevation Specific Technology to exactly match the unique irregularities of each individual eye.
The process begins with an EyePrint Impression, which captures the precise curvatures of the entire ocular surface. Doctors then send the resulting impression to an EyePrint lab for 3-D scanning.
The scanned data is then fed to a numerically controlled machining system to produce a lens that matches the impression exactly and therefore fits the individual cornea and sclera perfectly. Because of the precise nature of the back surface fit, high quality and individualized optics can be placed on the front surface of the device.
"The EyePrint is like a fingerprint—it's completely individual," says EyePrint developer Dr. Christine Sindt, Clinical Associate Professor of Ophthalmology and Visual Sciences at University of Iowa.
The EyePrintPRO can only be fit by doctors who undergo specific training and certification. To learn more and to find an eye doctor who prescribes and fit these prosthetic lenses, visit the EyePrint Prosthetics website.
8. Intacs
Intacs (Addition Technology) are FDA-approved clear, arc-shaped corneal inserts that are surgically positioned within the peripheral cornea to reshape the front surface of the eye for clearer vision.
Intacs may be needed when keratoconus patients no longer can obtain functional vision with contact lenses or eyeglasses.
Several studies show that Intacs can improve the best spectacle-corrected visual acuity (BSCVA) of a keratoconic eye by an average of two lines on a standard eye chart. The implants also have the advantage of being removable and exchangeable. The surgical procedure takes only about 10 minutes.
Intacs might delay but can't prevent a corneal transplant if keratoconus continues to progress.
9. Topography-guided conductive keratoplasty
While more study is needed, early results of a small study involving topography-guided conductive keratoplasty (CK) show this procedure might help smooth irregularities in the corneal surface.
This treatment uses energy from radio waves, applied with a small probe at several points in the periphery of the cornea to reshape the eye's front surface. A topographic "map" created by computer imaging of the eye's surface helps create individualized treatment plans.
SEE RELATED: What is corneal disease?
10. Corneal transplant
Some people with keratoconus can't tolerate a rigid contact lens, or they reach the point where contact lenses or other therapies no longer provide acceptable vision.
The last remedy to be considered may be a cornea transplant, also called a penetrating keratoplasty (PK or PKP). Even after a transplant, you most likely will need glasses or contact lenses for clear vision.
SEE RELATED: What Is Corneal Ectasia?