Glaucoma vs. macular degeneration
Glaucoma and age-related macular degeneration (AMD) are common eye conditions experienced by millions of people worldwide. While they typically impact different parts of the eye, both have the potential to cause significant vision loss and blindness.
What is macular degeneration?
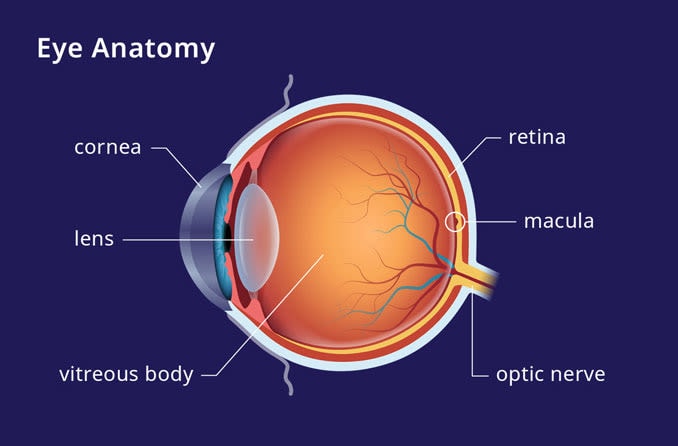
Macular degeneration affects the macula, the center part of the retina that is located in the back of the eye. The macula is responsible for your sharpest vision. Damage to the macula can lead to the loss of central vision, what you see when looking directly in front of you.
There are two primary types of age-related macular degeneration:
Dry AMD
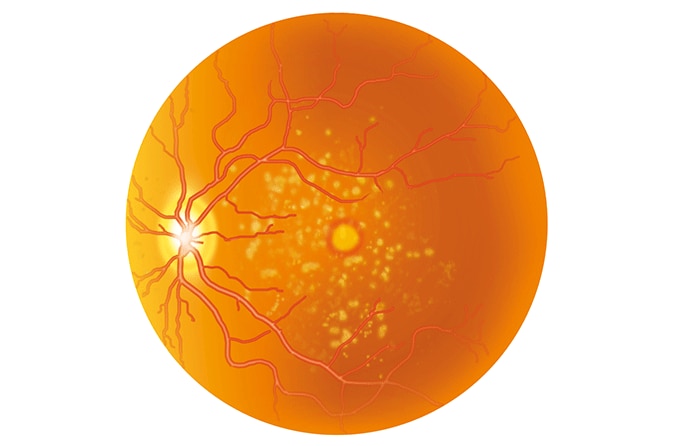
Dry AMD, also called atrophic AMD, is the more common form. It develops slowly over time and occurs when the macula thins and begins to break down. Small areas of drusen (a yellow deposit made of proteins and fats) also appear in the macula. (However, the presence of drusen does not always indicate macular degeneration.)
Wet AMD
Though less common, wet AMD progresses to vision loss more quickly. Also called neovascular AMD, it occurs when new, abnormal blood vessels develop in the retina. These vessels can leak blood or fluid, damaging the macula.
Macular degeneration symptoms
Macular degeneration may not cause any noticeable symptoms until the condition has progressed. When symptoms do appear, they vary based on the type of AMD.
Dry AMD symptoms include:
- Blurry or distorted central vision
- Difficulty seeing in dim lighting
- Changes in your color vision
- Difficulty seeing fine details, such as when reading or recognizing faces
Wet AMD symptoms include:
- Distorted or wavy central vision
- Straight lines appear wavy
- Blank or dark spots in your vision
- Difficulty seeing in dim lighting
- Changes in your color vision
- Difficulty seeing fine details, such as when reading or recognizing faces
Macular degeneration diagnosis
Signs of age-related macular degeneration are typically detected through a comprehensive eye exam. The following tests and techniques may be used to help diagnose the condition:
- Visual acuity test – Measures how well you can see at certain distances
- Amsler grid test – Screens for wavy, distorted or blank spots in your central vision
- Pupil dilation – Provides a wider view of your retina and macula
- Fluorescein angiography – Identifies leaky blood vessels in the retina
- Optical coherence tomography (OCT) – Detects drusen, fluid, abnormal blood vessels and other signs of AMD in the retina
Eye doctors may use additional tests and procedures to help confirm a macular degeneration diagnosis.
Macular degeneration treatment
Treatment for macular degeneration depends on the type of AMD present and other factors. Currently, there is no cure for the condition. However, prompt treatment may help delay or prevent further vision loss.
Dry AMD treatments
At this time, the options for treating early to moderate dry AMD are limited. Nutritional strategies, such as taking specific formulations of vitamins and minerals, may help lower the speed of disease progression.
An advanced form of dry AMD, known as geographic atrophy (GA), may be treated with the following injectable medications:
- Pegcetacoplan (Syfovre)
- Avacincaptad pegol (Izervay)
Wet AMD treatments
The initial treatment for wet AMD typically involves anti-vascular endothelial growth factor (anti-VEGF) medications. These are injected into the eye to help control the growth and leakage of new, abnormal blood vessels.
A wide variety of anti-VEGF medications may be used to treat wet AMD. Common options include:
Laser-based treatments may also be used to treat wet macular degeneration, including:
- Laser photocoagulation – Uses powerful laser light to seal leaking blood vessels in the macula
- Photodynamic therapy – Combines the use of a laser and intravenous medication to block leaking blood vessels
Both the early diagnosis and timely treatment of macular degeneration are key to preserving your eyesight and reducing your risk of vision loss.
What is glaucoma?
Glaucoma is a group of eye conditions that damage the optic nerve in the back of the eye. The optic nerve transmits visual information from the retina to the brain, allowing you to process and understand what you see. Damage to the optic nerve can cause permanent vision loss and blindness, especially without prompt treatment.
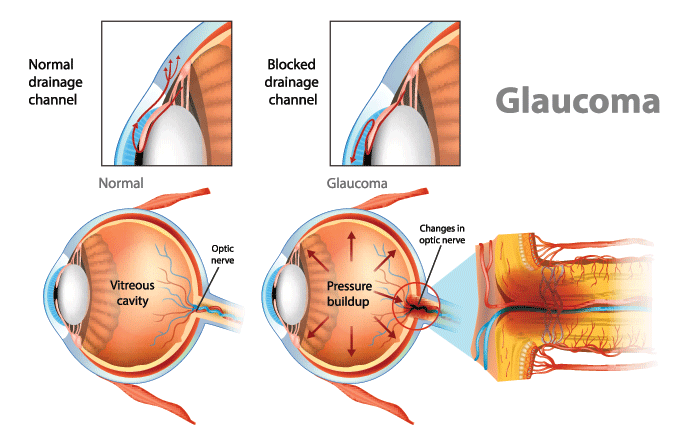
Glaucoma can result from several factors, but it is often associated with increased intraocular pressure (IOP), or high pressure inside the eye. This pressure buildup typically occurs when the aqueous humor — the fluid in the front of the eye — fails to drain properly through tiny canals called the trabecular meshwork. As fluid accumulates, the rising IOP can gradually harm the optic nerve.
While there are several different forms of glaucoma, the main types include:
- Open-angle glaucoma – The drainage angle, located where your iris (the colored part of your eye) and the sclera (the white of your eye) meet, remains open. However, fluid doesn’t drain properly.
- Angle-closure glaucoma – The drainage angle is too narrow or becomes blocked, causing fluid to build up quickly.
- Congenital glaucoma – The drainage system doesn’t form correctly during fetal development, causing a person to be born with glaucoma.
- Secondary glaucoma – This develops when other conditions or factors (such as injuries or medications) cause increased IOP.
Open-angle glaucoma is the most common type.
LEARN MORE about the types and causes of glaucoma
Glaucoma symptoms
Glaucoma typically has no noticeable symptoms in the early stages, especially in cases of open-angle glaucoma. As the disease develops, symptoms such as peripheral (side) vision loss may occur gradually.
Certain types of glaucoma, including angle-closure, can cause a sudden (acute) onset of symptoms, including:
- Intense eye or forehead pain
- Eye redness
- Blurry vision
- A partially dilated pupil that does not respond to light
- Seeing multicolored halos around lights
- Nausea
- Vomiting
- Headache
The abrupt appearance of glaucoma symptoms is a medical emergency. If you experience any glaucoma symptoms, seek medical care immediately.
Glaucoma diagnosis
Detecting glaucoma begins with a comprehensive eye exam. Specific tests and techniques for diagnosing glaucoma include:
- Tonometry – Measures the pressure within the eye (IOP)
- Visual field test – Evaluates peripheral vision
- Pupil dilation – Provides a clear view of the optic nerve
- Pachymetry – Measures the thickness of the cornea (the clear front surface of the eye)
- Gonioscopy – Assesses the drainage angle and trabecular meshwork
- Optic nerve imaging – Uses a technique like optical coherence tomography to evaluate for optic nerve damage
Routine eye exams are important for catching glaucoma as early as possible.
Glaucoma treatment
The early diagnosis and timely treatment of glaucoma are key to preserving your eyesight and reducing your risk of vision loss. Treatment strategies vary according to the type of glaucoma you have. However, treatment typically focuses on lowering eye pressure.
Glaucoma treatment options may include:
- Eye drops – Prescribed to help lower and control IOP
- Laser procedures – Performed to drain eye fluid
- Surgery – Performed to improve fluid drainage in the front of the eye
Key differences between macular degeneration and glaucoma
Macular degeneration and glaucoma both have the potential to lead to vision loss and blindness. However, they each impact the eye and vision in different ways. Some of the key differences between these conditions include:
How the eye is affected
Macular degeneration involves the deterioration of the macula. It can lead to central vision loss but usually does not affect peripheral vision.
Glaucoma damages the optic nerve, often in conjunction with high intraocular pressure. It leads to peripheral vision loss that can progress to complete vision loss if left untreated.
Possible symptoms
Both macular degeneration and glaucoma may not cause symptoms in the early stages. However, symptoms may occur as each condition progresses.
Macular degeneration causes symptoms such as:
- Blurry, distorted or wavy central vision
- Dark or blank spots in your vision
- Difficulty seeing fine details
Glaucoma causes symptoms such as peripheral vision loss. Acute cases or “attacks” may suddenly cause symptoms such as:
- Eye pain
- Blurry vision
- Rainbow-colored rings around lights
- Nausea, vomiting or headache
A sudden onset of glaucoma symptoms is a medical emergency. Seek medical care right away if you notice any new glaucoma symptoms.
How vision loss can occur
With macular degeneration, central vision loss occurs as the macula deteriorates. This affects the ability to see fine details and perform everyday activities, such as reading, watching television and driving.
Glaucoma damages the optic nerve, often due to increased eye pressure. This damage can cause peripheral vision loss, affecting what you see out of the corners of your eyes. As the disease advances, central vision loss and complete blindness can also occur.
Risk factors
Glaucoma and macular degeneration can affect anyone. However, certain factors can increase the likelihood of developing these conditions.
Macular degeneration risk factors include:
- Age – AMD typically affects people aged 50 and older.
- Genetics – A genetic predisposition (and family history) can increase your risk of developing the disease.
- Ethnicity – Non-Hispanic white individuals experience AMD more than other racial groups.
- Sex – Women have a higher risk of experiencing the condition than men.
- Health factors – Certain health problems, such as high blood pressure and obesity, can raise the risk of developing macular degeneration.
- Lifestyle factors – Smoking, a poor diet and inadequate amounts of exercise can also contribute to the development of AMD.
Glaucoma risk factors can vary according to glaucoma type. Common risk factors include:
- Age – In the general population, glaucoma is most likely to affect people over the age of 60. For African Americans, that risk increases after age 40.
- Race – Angle-closure glaucoma is more prevalent among Native Alaskans and Asians. Another type, called low-tension glaucoma, is more common in people of Japanese ancestry.
- Genetics – A family history of glaucoma can increase your risk of developing the disease.
- Health factors – Certain systemic conditions, such as high blood pressure, heart problems and diabetes, can increase your glaucoma risk.
- Eye trauma – Eye damage or injuries that lead to increased eye pressure can also be a risk factor.
- Eye anatomy – The shape of the eye and its structures, such as the cornea, can raise the risk of experiencing the condition.
- Steroid use – The prolonged use of corticosteroids may increase the chance of developing secondary glaucoma.
How they're managed
Managing macular degeneration involves slowing or preventing:
- The deterioration of the macula
- The growth of new, abnormal blood vessels in the retina
Treatments vary according to the type of AMD present. They may involve:
- Dietary supplements
- Injected eye medications
- Laser procedures
Glaucoma management focuses on reducing intraocular pressure and slowing or preventing disease progression. Treatments vary depending on the type and may include:
- Prescription eye drops
- Laser procedures
- Glaucoma surgery
Key similarities between glaucoma and macular degeneration
Glaucoma and macular degeneration are two unrelated conditions affecting different parts of the eye. However, they share some similarities in terms of prevention, risk of vision loss and how they’re detected.
Prevention
Protecting your eye and vision health from conditions such as macular degeneration and glaucoma involves factors such as:
- Eating a balanced diet
- Getting regular exercise
- Quitting or avoiding smoking
- Maintaining good general health
The possibility of vision loss
Both conditions can impact your sight in some way. They can also result in permanent vision loss without treatment.
Macular degeneration can lead to central vision loss, but it will not cause complete blindness.
Glaucoma initially causes peripheral vision loss, but it can progress to affect central vision and may eventually cause complete blindness.
The importance of routine eye exams
The early diagnosis of macular degeneration and glaucoma is key to preserving your vision. Getting an eye exam once a year gives your eye doctor opportunity to detect these vision-threatening conditions before obvious symptoms appear.
Routine eye exams also allow your eye doctor to identify risk factors you may have, monitor your eyes and vision for changes, and determine treatment strategies.
If you’re due for an eye exam or you’ve noticed any changes in your vision, contact an eye doctor near you to schedule an exam.
READ NEXT: How vision changes as you age