What is an occipital seizure?
An occipital seizure is a seizure that begins in the occipital lobe of the brain, where visual information is processed. It is a characteristic of occipital lobe epilepsy, a rare condition in which recurrent seizures cause visual symptoms and other effects.
A seizure occurs when a burst of unusual electrical activity in the brain disrupts normal nerve cell function. It can present in various ways, from convulsions to altered sensory perception. Generalized seizures affect both sides of the brain, while focal seizures start in one part of the brain.
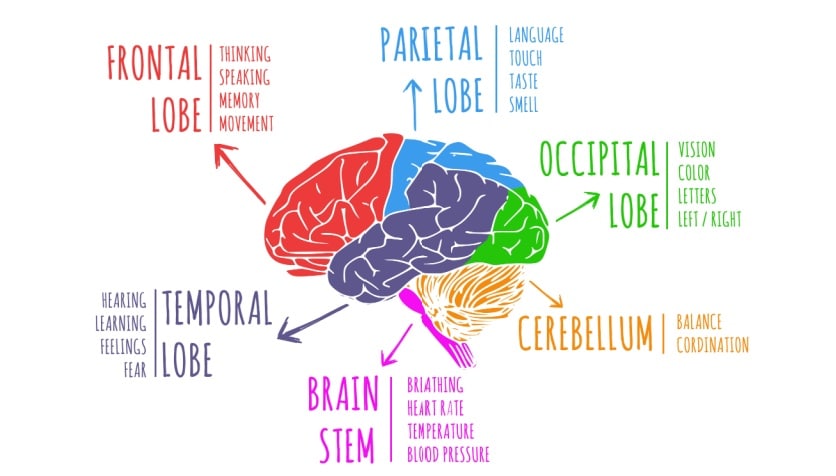
Focal epilepsy types are classified based on where in the brain the abnormal activity begins. The brain has four lobes, each responsible for specific functions:
- Frontal lobe – Memory, speech, language, emotions and personality
- Parietal lobe – Sensory processing (of pain and pressure for example), motor functions, learning, language and spatial recognition
- Temporal lobe – Auditory (sound) processing, memory, and visual and facial recognition
- Occipital lobe – Visual processing and interpretation
Seizures that begin in the occipital lobe can migrate to affect other parts of the brain, which may cause additional symptoms.
Occipital epilepsies account for 5% to 10% of all epileptic conditions. While they can occur at any age, they are most common in childhood.
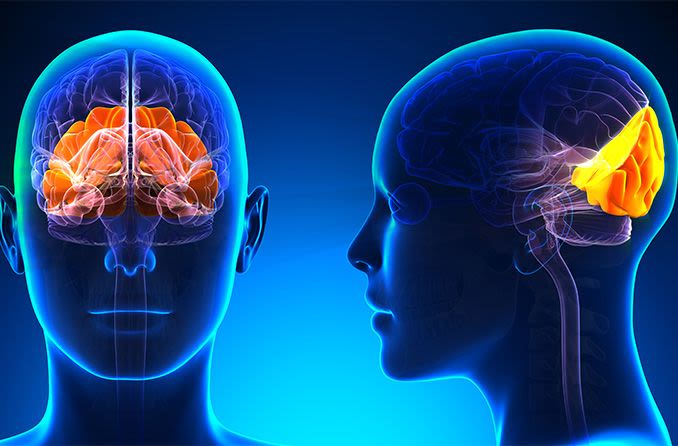
The occipital lobe and vision
The occipital lobe is the smallest lobe of the brain. It is located in the back of the head, just above the occipital bone at the base of the skull.
The occipital lobe houses the visual cortex, which controls how you process and interpret the information you see. Once visual information is analyzed, it is sent to other areas of the brain for further interpretation.
The occipital lobe is responsible for the following functions:
- Visual memory formation
- Face and object recognition
- Color perception and processing
- Depth and distance perception
- Spatial processing (allowing you to see texture and shapes)
LEARN MORE: How does the brain control eyesight?
Eye seizure vs. migraine with aura
Occipital lobe seizures are sometimes referred to as “eye seizures.” They are often mistaken for migraines with aura because of their similar symptoms. (Learn more about symptoms in the next section.) Migraines with aura are headaches preceded by sensory phenomena or motor disruptions, such as tingling on one side of the body.
Occipital seizures and migraines with aura share many of the same visual symptoms, including visual hallucinations. This is a key reason they are often confused. However, there are some distinct differences between these two conditions:
- Onset – Occipital seizures typically have a sudden onset. Migraines with aura develop more gradually.
- Duration – Occipital seizures typically last less than two minutes. Migraine auras usually last between five and 60 minutes before headache pain sets in.
Doctors may perform medical tests and procedures to determine an accurate diagnosis.
SEE RELATED: What is an ocular migraine?
Occipital seizure symptoms
Occipital seizures can cause a variety of symptoms that impact vision and other bodily functions. Symptoms may occur on one side of the visual field, depending on which side of the brain is affected:
- Right-sided seizures affect the left visual field.
- Left-sided seizures affect the right visual field.
Visual occipital epilepsy symptoms can include:
- Flashing bright lights (often multicolored and circle-shaped)
- Visual hallucinations
- Horizontal eye deviation
- Blurred vision
- Vision loss
- Blindness
- Palinopsia (continuing to see an image that’s no longer in your visual field, even after a significant delay)
- Polyopia (perceiving multiple images of a single object)
- Nystagmus (repetitive, uncontrolled eye movement)
- Eyelid fluttering
- Scotomas (blind spots in your visual field)
- Macropsia (objects look larger than their actual size)
- Micropsia (objects look smaller than their actual size)
- Metamorphopsia (objects seem to have a distorted shape)
- Enlarged (“blown”) pupils
Non-visual symptoms often involve:
- Convulsions
- Headaches
- Nausea and vomiting
- Vertigo
- Tinnitus (ringing in the ear)
- Ear pain
SEE RELATED: What is Alice in Wonderland syndrome?
Causes and risk factors for occipital lobe epilepsy
Occipital lobe epilepsy can occur in different forms. Various factors can contribute to or increase the risk of experiencing this condition, including:
Idiopathic causes
Some types of occipital epilepsy may be “idiopathic,” meaning the cause is unknown. Seizures may occur spontaneously or be triggered by environmental factors, such as flashing lights from digital screens or televisions. Genetic factors may also play a role in a person’s risk for these types of epilepsies.
Genetic disorders
Certain inherited conditions can increase the risk of experiencing occipital seizures. These include various forms of mitochondrial diseases and epilepsy syndromes.
Brain abnormalities
Brain abnormalities can contribute to occipital epilepsy and may result from:
- Congenital disorders (those present at birth)
- Vascular malformations in the brain
- Abnormalities in brain development
- Tumors or lesions in or near the occipital lobe
- Traumatic brain injuries
Metabolic conditions
People with certain metabolic conditions, such as celiac disease, are more likely to develop occipital epilepsy.
Other factors
Occipital seizures are sometimes triggered by external factors, including:
- Bright or flashing lights, including those on screens and in certain medical tests
- Sleep deprivation
- Drug or alcohol use
- Long periods of digital gaming
Occipital epilepsy diagnosis
Diagnosing occipital epilepsy typically begins with reviewing seizure symptoms. Neuroimaging tests, such as the following, may also be performed:
- Electroencephalogram (EEG) – Measures electrical activity in the brain
- Magnetic resonance imaging (MRI) – Provides detailed images of the brain
- Computed tomography (CT) scans – Reveals structural information about the brain
These tests allow doctors to screen for and evaluate brain abnormalities that may indicate the presence of epilepsy.
Occipital seizure treatment and management
Occipital seizures may be managed through a variety of treatment options, which are often determined based on the cause, type and severity of the condition. While some forms of occipital lobe epilepsy do not require treatment, others are managed through the following methods:
Medication
Treating occipital seizures typically involves one or more of the following anti-seizure medications:
- Carbamazepine (Carbatrol, Tegretol, Equetro, Epitol)
- Oxcarbazepine (Trileptal)
- Levetiracetam (Keppra)
- Lamotrigine (Lamictal, Subvenite)
- Valproic acid (Depakene)
- Sodium valproate (Depacon)
- Phenobarbital (Luminal, Solfoton)
- Topiramate (Topamax)
- Zonisamide (Zonegran)
- Clonazepam (Klonopin)
Most occipital lobe epilepsies resolve within two to five years after onset. Some patients can stop taking anti-seizure medication after a period of being seizure-free. However, others may require lifelong medication to manage the condition.
Surgical intervention
Surgery may be performed in certain cases of occipital epilepsy, particularly when:
- Medications are not effective at controlling the seizures
- The seizures are due to a growth or lesion in the brain
Diet and lifestyle changes
Treating occipital lobe seizures may also involve adopting certain lifestyle adjustments. For instance, a gluten-free diet may help control celiac-related occipital epilepsies. A ketogenic diet — high in fats and low in carbohydrates — may be recommended for some children.
Lifestyle changes may also include trigger avoidance. For example, it may help to avoid factors that could potentially trigger seizures, such as:
- Flashing lights
- Sleep deprivation
- Extended screen use (including TV and video games)
- Drug and alcohol use
- Poor nutrition
- Stress
- Missed doses of medication
When to see a doctor
Occipital lobe epilepsy can impact your vision and quality of life in several ways. It can cause occipital seizures that may lead to visual hallucinations, abnormal eye movements and other effects.
If you or your child experiences any visual symptoms, schedule an eye exam with your eye doctor as soon as possible. They may refer you to a neurologist or other specialist for further assessment and treatment. Early diagnosis and care are key to protecting your health and managing the condition.
READ NEXT: Does losing your vision make your other senses stronger?